Nocturnal enuresis in adults
Contents
Nocturnal enuresis (NE) is the involuntary voiding of urine during sleep. Studies show that at least 2% of adults have a lack of control of urination during the night. Nocturnal enuresis is not to be confused with nocturia or waking two or more times per night to void. Different types of enuresis exist, which need to be differentiated.
Persistent Primary Nocturnal Enuresis is a condition that begins during childhood, where nighttime dryness has not been achieved for longer than six months. About 2-3% of male and female adults that are older than 18 years of age have this type of nocturnal enuresis. Adult Onset Secondary Enuresis is defined as nocturnal enuresis in which nighttime dryness is achieved at some point in life and, for some, dryness may have occurred for years, but nighttime wetting begins at an older age.
Nocturnal enuresis has affected people for many years. Evidence of this problem can be traced back as far as 1500 BC. While extensive research has been devoted to nocturnal enuresis in children, persistent primary enuresis and adult onset secondary enuresis in particular have not been studied as thoroughly. It must be understood that bedwetting is unintentional and is not something that can be voluntarily controlled at any age.
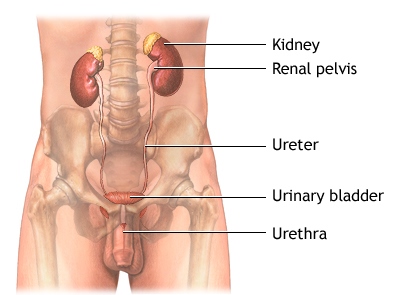
To begin, a discussion of the anatomy and bladder function will be helpful. Urine is produced by the kidneys and travels through the ureters to the bladder to be stored. The bladder is a muscular sac that holds urine until it is ready to be released into the urethra, the tube that connects the bladder to the outside of the body. The bladder is emptied when the detrusor muscle, the muscle within the bladder wall, contracts thereby squeezing urine out of the body. At the same time the bladder contracts, the urinary sphincter relaxes. The relaxed sphincter acts like an open door, which allows the urine to pass and exit the body. For successful urination, both the detrusor muscle contraction and sphincter relaxation must occur simultaneously. Nerves in the muscular wall of the bladder release acetylcholine [uh-seet-l-koh-leen], a chemical that attaches to receptors on the muscle cells causing them to contract. Signals from the nerves are sent to the cortex of the brain communicating that it is time to be emptied. This process is primarily autonomic, which is not a voluntary control. Overall, the normal communication between different nerves, muscles, and the brain is very complicated.
The reason nocturnal enuresis occurs in adults is thought to be attributed to multiple factors. A large percentage of adults have significant symptoms associated with bedwetting and may have daytime wetting as well. It is important to recognize these symptoms associated with nocturnal enuresis, as they may indicate a urological disorder.
Firstly, nocturnal enuresis can occur due to genetic linkage. Though this is not true with all people, evidence has shown that bedwetting is hereditary. One study has shown that someone with two bedwetting parents has a 77% chance of becoming a bedwetter. When one parent wet the bed as a child, his son or daughter was found to have a 40% chance of becoming a bedwetter. These probabilities carry into adulthood as well.
ADH, or antidiuretic [an-tee-dahy-uh-ret-ik] hormone, is a signaling hormone that tells the kidneys to decrease the amount of urine produced. Normally the body produces more ADH at night causing the kidneys to produce less urine. Decreased urine production at night allows people to sleep through the night without having to urinate. However, some people do not produce the appropriate amount of this hormone at night, which leads to high production of urine. This is very similar to a symptom related with Type II Diabetes where an ineffective amount of ADH is produced. In other cases, the body produces ADH, but the kidneys do not respond and continue to produce the same amount of urine. This abnormality is defined as nocturnal polyuria, the excessive production of urine during sleep, which can cause nocturnal enuresis in adults. It can also be a symptom related to Type I Diabetes. Since similar symptoms can be shared by individuals with different conditions. Consulting a healthcare professional is helpful especially if you feel that you may be experiencing diabetes or nocturnal enuresis.
Another cause cited for primary nocturnal enuresis is a “smaller” bladder. This does not mean, however, that the physical size of the bladder is actually smaller in nocturnal enuresis patients than in their peers. Instead, it means that their functional bladder capacity (FBC), the amount of urine the bladder will hold until sending a signal to the brain indicating it is time to urinate, is a smaller volume than that of their peers. The overactive contractions of the detrusor muscle indicate that the muscle is never fully relaxed and therefore the bladder capacity is not as large.
Along with FBC, detrusor overactivity, or instability, can also cause nocturnal enuresis. Detrusor overactivity is spontaneous detrusor muscle contractions that may cause accidents. Many studies have found a high incidence of detrusor instability with nocturnal enuresis. Detrusor overactivity has been found in up to 70-80% of primary nocturnal enuresis patients. Bladder irritants, such as alcohol and caffeine, can also contribute to detrusor instability, in addition to serving as diuretics that only increase urine production.
Some medications have been documented to cause nocturnal enuresis as a side effect including hypnotics or medications taken for insomnia and drugs taken for psychiatric purposes. Obstructive sleep apnea or sleep disorders can cause nocturnal enuresis as well. Be sure to talk to your healthcare provider about any medications prescribed and their side effects. Much research supports the belief that secondary enuresis in adults is usually a serious symptom of an underlying problem that should be investigated. Generally, this type of bedwetting occurs with other symptoms and is often associated with daytime wetting. Adult onset nocturnal enuresis is often a result of problems with the urethra, such as prostatic or primary vesicle neck obstruction. Such problems can be associated with the prostate in men or pelvic organ prolapse in women.
Additional causes of secondary enuresis may also include diabetes, urinary tract infection, urinary tract stones, neurological disorders, anatomical abnormalities, urinary tract calculi, prostate cancer, prostate enlargement, bladder cancer, and obstructive sleep apnea. In very rare cases, acute anxiety or emotional disorder may cause adult bedwetting.
One of the most useful tools for a healthcare provider is to have a great deal of information about your symptoms and general habits. Consider keeping a symptom diary of daily habits and routines for at least two days prior to a medical appointment. These details will assist your healthcare provider when determining the cause and severity.
Take care to note when you void during the day and night
- When accidents occur (time of day or night)
- Amount of urine voided
- Drinking patterns (do you drink a lot of fluids in the later afternoon/evening?)
- What you drink (sugary, caffeinated, artificially sweetened, carbonated, alcoholic drinks, etc.)
- Nature of the urinary stream (is the urinary stream strong and constant or is there difficulty initiating a void or continuous dribbling?)
- Any existing recurrent urinary tract infections
- The number of wet versus dry nights
In addition, note any other symptoms associated with nocturnal enuresis such as night sweats
Any and all of this information can help a healthcare provider determine the cause of the problem and the appropriate treatment.
At the time of the appointment, you should be prepared to supply such information and details related to personal and family medical history as well as medication usage. In addition to helping you find options to help cure bedwetting, it is also important to see a healthcare provider to rule out any other serious problems that may cause nocturnal enuresis as a side effect.
At the appointment you can expect:
- A physical examination
- Neurological evaluation
Urinalysis and urine culture: The urinalysis and urine culture are different tests that determine the contents of the urine.
Further tests include:
- Uroflowometry: involves urinating into a specialized funnel that measures the flow rate, amount of urine, and time required for urination
- Post-void residual urine measurements: require an ultrasound and are non-invasive procedures that determine the volume of urine left in the bladder after voiding
If other problems are suspected, you can expect further tests for diagnosis.
For those suffering from persistent primary nocturnal enuresis, many treatments can be used at any age.
Pharmacological Therapy
Different medicinal options exist to treat nocturnal enuresis. These may be used alone or combined with some of the behavioral treatments listed above, which generally has proven to be more effective. Many studies have shown, however, that while pharmacological treatment may be initially effective in lowering the number of wet nights, the medicine is often effective only as long as it is taken. In other words, relapse rates are high once treatment has stopped, as only symptoms are addressed by the medication rather than the underlying condition or causal factors. The professional medical advice of a healthcare provider should be sought before starting any of these treatments.
Surgical Methods
The involvement of surgery when attempting to treat severe detrusor overactivity is limited and should only be considered when all other less invasive treatment options have proven to be unsuccessful. All of the procedures mentioned below have associated risks that must be considered and discussed with a healthcare professional.
Options to help manage bedwetting during treatment exist.
Mattress Covers: A variety of products exist to protect the bed including vinyl, waterproof, and absorbing mattress covers or even sheet protectors, which can make clean-up easier.
Absorbent Briefs: These products are a form of modified underwear designed to absorb liquid, therefore preventing leakage. Both reusable and disposable products are available. For those prone to skin irritation, disposable types may be a better option.
Skincare Products: Many products exist to protect the skin from irritation and soreness that occur when a person experiences nocturnal enuresis. A range of soaps, lotions, and cleansing cloths exist for various skin types.
Source: http://www.nafc.org/bladder-bowel-health/bedwetting-2/adult-bedwetting/

