Stable angina
Stable angina is chest pain or discomfort that usually occurs with activity or stress. Angina is chest discomfort due to poor blood flow through the blood vessels in the heart.
CAUSES
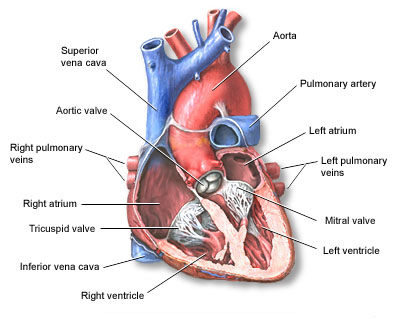
Your heart muscle is working all the time, so it needs a constant supply of oxygen. This oxygen is provided by the coronary arteries, which carry blood.
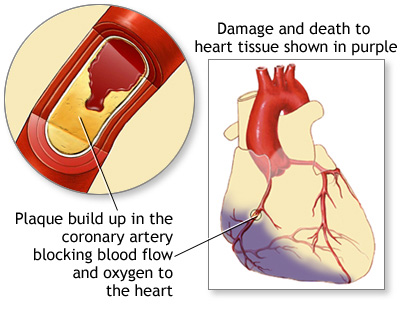
When the heart muscle has to work harder, it needs more oxygen. Symptoms of angina occur when the coronary arteries are narrowed or blocked by hardening of the arteries (atherosclerosis), or by a blood clot.
The most common cause of angina is coronary heart disease (CHD). Angina pectoris is the medical term for this type of chest pain.
Stable angina is less serious than unstable angina, but it can be very painful or uncomfortable.
There are many risk factors for coronary heart disease. Some include:
- Diabetes
- High blood pressure
- High LDL cholesterol and low HDL cholesterol
- Smoking
Anything that makes the heart muscle need more oxygen can cause an angina attack in someone with heart disease, including:
- Cold weather
- Exercise
- Emotional stress
- Large meals
Other causes of angina include:
- Abnormal heart rhythms (usually ones that cause your heart to beat quickly)
- Anemia
- Coronary artery spasm (also called Prinzmetal's angina)
- Heart failure
- Heart valve disease
- Hyperthyroidism (overactive thyroid)
SYMPTOMS
Symptoms of stable angina are most often predictable. This means that the same amount of exercise or activity may cause your angina to occur. Your angina should improve or go away when you stop or slow down the exercise.
The most common symptom is chest pain that occurs behind the breastbone or slightly to the left of it. The pain of stable angina usually begins slowly and gets worse over the next few minutes before going away.
The pain may feel like tightness, heavy pressure, squeezing, or crushing pain. It may spread to the:
- Arm (usually the left)
- Back
- Jaw
- Neck
- Shoulder
Some people say the pain feels like gas or indigestion.
Some patients (women, older adults, and people with diabetes) may have different symptoms, such as:
- Back, arm, or neck pain
- Fatigue
- Shortness of breath
- Weakness
The pain of stable angina usually:
- Occurs after activity or stress
- Lasts an average of 1 - 15 minutes
- Is relieved with rest or a medicine called nitroglycerin
Angina attacks can occur at any time during the day, but a higher number occur between 6 a.m. and noon.
Other symptoms of angina include:
- A feeling of indigestion or heartburn
- Dizziness or light-headedness
- Nausea, vomiting, and sweating
- Palpitations
- Shortness of breath
- Unexplained tiredness after activity (more common in women)
EXAMS AND TESTS
Your doctor or nurse will examine you and measure your blood pressure. Tests that may be done include:
- Coronary angiography
- Coronary risk profile (special blood tests)
- ECG
- Exercise tolerance test (stress test or treadmill test)
- Stress echocardiogram
TREATMENT
The options for treating angina include lifestyle changes, medications, and procedures such as coronaryangioplasty with stent placement or coronary artery bypass surgery.
You and your doctor should agree on a plan for treating your angina on a daily basis. This should include:
- What medicines you should be taking to prevent angina
- What activities are okay for you to do, and which ones are not
- What medicines you should take when you have angina
- What are the signs that your angina is getting worse
- When you should call the doctor or 911
MEDICATIONS
You may be asked to take one or more medicines to treat blood pressure, diabetes, or high cholesterol levels. Follow your doctor's directions closely to help prevent your angina from getting worse.
Nitroglycerin pills or spray may be used to stop chest pain.
Taking aspirin and clopidogrel helps prevent blood clots from forming in your arteries, and reduces your risk of having a heart attack. Ask your doctor whether you should be taking these medications.
Your doctor may give you one or more medicines to help prevent you from having angina.
- ACE inhibitors to lower blood pressure and protect your heart
- Beta-blockers to lower heart rate, blood pressure, and oxygen use by the heart
- Calcium channel blockers to relax arteries, lower blood pressure, and reduce strain on the heart
- Nitrates to help prevent angina
- Ranolazine (Ranexa) to treat chronic angina
NEVER STOP TAKING ANY OF THESE DRUGS ON YOUR OWN. Always talk to your doctor first. Stopping these drugs suddenly can make your angina worse or cause a heart attack. This is especially true of anti-clotting drugs (aspirin, clopidogrel).
Your doctor may recommend a cardiac rehabilitation program to help improve your heart's fitness.
SURGICAL TREATMENT
Some people will be treated with medicines and will not need surgery to treat a blockage or narrowing. Others will need a procedure to open narrowed or blocked blood vessels that supply blood to the heart.
- Angioplasty and stent placement (also called percutaneous coronary intervention)
- Blockages that cannot be treated with angioplasty may need a heart bypass
PROGNOSIS
Stable angina usually improves with medication.
WHEN TO CONTACT A DOCTOR
Seek medical attention if you have new, unexplained chest pain or pressure. If you have had angina before, call your doctor.
Call emergency if your angina pain:
- Is not better 5 minutes after you take nitroglycerin
- Does not go away after three doses of nitroglycerin
- Is getting worse
- Returns after the nitroglycerin helped at first
Call your doctor if:
- You are having angina symptoms more often
- You are having angina when you are sitting (rest angina)
- You are feeling tired more often
- You are feeling faint or light-headed
- Your heart is beating very slowly (less than 60 beats a minute) or very fast (more than 120 beats a minute), or it is not steady
- You are having trouble taking your heart medicines
- You have any other unusual symptoms
Seek medical help right away if a person with angina loses consciousness.
PREVENTION
A risk factor is something about you that increases your chance of getting a disease or having a certain health condition.
Some risk factors for heart disease you cannot change, but some you can. Changing the risk factors that you can control will help you live a longer, healthier life.
Source: http://www.nlm.nih.gov/medlineplus/ency/article/000198.htm

